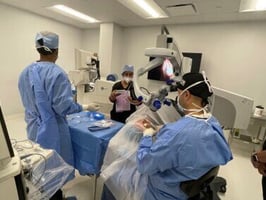
Move to Office-Based Surgery With few Ambulatory Surgery Centers (ASCs) in northern Virginia, John...
Training Staff and Managing Expectations for Improved Productivity
Over the last few years, my ophthalmology practice began encountering some of the challenges that typically drive surgeons toward office-based surgery (OBS). We noticed increasing difficulty scheduling OR time at the hospital or ambulatory surgery centers (ASCs) where we operated. When we would reserve two adjacent rooms for a procedure, one room might get bumped with little notice. Accommodating patient requests for specific surgical times became nearly impossible. And of course, the COVID-19 pandemic exacerbated those problems and generated many more. For those reasons, we pursued office-based cataract surgery as an alternative, better way to care for our patients.
Since we transitioned, I’ve seen a rapid increase in efficiency, particularly as our staff continues to learn and gain expertise in caring for the surgical patients in our suite. At this point, I feel we are just as efficient, if not more so than a two-room ASC.
Optimizing Workflow in the OBS
Improving the flow of patients through the practice was a primary goal. Training our staff became the most important factor in getting there. They had experience in office settings, but not in surgical ones. We learned that not all our staff members were ideally suited for the surgical suite. Some work better in the office setting and others seem born for the OR. The key is to identify the different strengths among staff members and apply them where they will work best. Thankfully, sorting that out in my practice was a short process.
Our second tactic was to set up realistic but achievable goals. From the beginning, we set the expectation for a benchmark of four cases per hour. Through very specific training and close monitoring, especially early in the process, we ensure that each staff member understands the job and discharges it correctly and effectively. A surgical suite functions efficiently only if everyone works as a team, with all members fully capable in their roles.
Staff Training

To save time and maximize productivity in getting our staff up to speed in their new roles, we worked with iOR Partners, which conducted most of the training. Their experts trained our office staff to an extremely high level of proficiency in office-based cataract surgery. As the process began, I was a bit skeptical that such a feat was possible, but iOR did an amazingly thorough job. They brought our staff to the point where I see continual improvement as their experience grows.
Excellent training is fundamental, but the key for us was to identify the staff members who are a good fit for the roles to be filled. For example, a circulator must focus on sterile and non-sterile areas, care for the patient, keep track of the surgery’s progress and respond immediately if needed. The pre-op/post-op person needs a different set of qualities: ideally, a calm, relaxed personality and the ability to engage patients in light conversation and transmit clear instructions at discharge time. On a hunch, we swapped roles between our circulator and pre-op/post-op person and found that our efficiency improved dramatically, with a commensurate rise in both staff members’ job satisfaction.
Staffing Guidelines
This experience revealed some general recommendations that can help a practice adapt to the new roles required for novel office-based cataract surgery. In less than four months, these guidelines helped us settle into our new grooves and reduce our average case time to just 15 minutes.
- Naturally, talkative staff often do better in pre/post roles, chatting with patients to keep them informed and reassured. Staff who may be less talkative and more task-focused tend to excel in the operating room.
- Pre-op and post-op people can be more relaxed types, which helps patients remain calm.
- Your scrub technician will benefit from a cool demeanor and the ability to quickly and calmly adapt to dynamic surgical situations.
- A circulator should be focused and detail-oriented.
- Train your staff for safety first, and then adjust for efficiency.
- Don’t be afraid to change roles and mix things up a bit, but give people some time to adjust. In my experience, the role changes were a great benefit.

Results
We currently operate just once a week, typically handling 15 to 20 cases from about 7:30 am to 1 pm with a break in-between. To increase our volume, perhaps to a 25-case maximum, we may break the operating day into morning and afternoon sessions.
For cataract cases, we averaged about four per hour in the ASC. It is nearly the same now in our OBS suite. Our surgery time is a little slower now than in the ASC, by about two minutes on average. That is due to our surgical scrubs and circulators having only three months’ experience, as opposed to the staff at the ASC with more than 20 years in the cataract surgery OR.
Our times have only been improving. I suspect that in a few months, I may be crowing about being more efficient and safer in my own iOR suite than in the ASC. This would be no surprise because an inherent benefit of our OBS is that the surgical staff only need to learn my preferences and techniques, not those of the 10 or more other surgeons who use the ASC. This will undoubtedly lead to increasing surgical-team cohesion and efficiency.
Likewise, OBS suites are smaller than those in ASCs. Everything is closer at hand and patients don’t need to be moved around as much. In ours, we do not conduct consecutive start-to-finish procedures in one room. We begin prepping the next patient in a separate room while we finish cleaning the current patient’s room. This further speeds up turnaround times, and is the sort of small improvement that can add up to big efficiencies for those willing to put in the work, drive the process and demand results.
Recommendations
With an OBS facility, keeping your focus on efficiency is a business and medical imperative. So is finding the right personnel for each role, guiding them to function as needed and motivating them to reach realistic performance and development goals.
Staff must understand the concept that everything needs to move in conjunction in a smooth workflow, almost like a ballet. When the surgery is over, the surgical scrub begins cleaning the table and hands the trays to the sterilizing technician. At the same time, the circulator brings the first patient to discharge, then the second patient into the OR. Smooth, efficient, and seamless.
As a pro tip for office-based cataract surgery, I recommend scheduling more difficult or lengthy cases toward the end of the surgical day, after you’ve warmed up and established a record of success with the easier procedures. Do not get discouraged if your new OBS suite isn’t humming along immediately. Give it some time, find out where the bottlenecks are, and fix them. With a patient and persistent commitment to continuous improvement along with well-trained staff who are well suited to their roles, you can expect to enjoy the benefits of OBS for many years to come.

Owner of Bluegrass Eyecare Center
Member, AAO, ASRS, and ASCRS